Aligning Your Benefits Package With Your Mission, Vision, and Values
Audio Overview:
Your company’s mission statement hangs in the lobby. Your values show up in onboarding decks and investor pitches, but when an employee opens their benefits portal during enrollment season, do those words mean anything?
For most mid-sized companies, the honest answer is no. Benefits decisions happen in a separate universe from brand strategy—driven by renewal deadlines, budget constraints, and whatever the broker recommends. The result is a disconnect between what you say you stand for and what you offer the people who make your business run.
That gap isn’t just philosophical. It’s a talent problem, a retention problem, and increasingly a credibility problem. Aligning your values-based employee benefits strategy with your mission doesn’t require unlimited budget. It requires intentionality, cross-functional conversation, and a willingness to treat benefits as infrastructure—not just an annual checkbox.
Why Mission-Aligned Benefits Matter More Than Ever
Benefits used to be table stakes—health insurance, a 401(k), maybe dental. Employees expected them, but they weren’t a differentiator. That’s changed.
According to SHRM’s 2025 Employee Benefits Survey, healthcare remains the benefit category employers are most likely to rate as extremely or very important for their workforce (89%), with leave benefits and retirement savings tied for second at 81% [1]. The menu of available benefits has expanded dramatically—SHRM now tracks over 200 distinct offerings—which means the choices you make about which benefits to provide increasingly signal what you actually prioritize.
Talent acquisition is values-driven. Glassdoor’s research found that 77% of adults would consider a company’s culture before applying for a job, and 73% wouldn’t apply at all unless their values aligned with the employer’s [2]. Benefits are one of the most tangible expressions of culture. If your mission emphasizes flexibility but your benefits require rigid in-office attendance for eligibility, you’ve created cognitive dissonance before day one.
Retention depends on trust. MetLife’s 2025 Employee Benefit Trends Study found that employees who both trust and feel cared for by their employer are 3.8 times more likely to feel holistically healthy, 2.4 times more likely to feel engaged, and 1.9 times more likely to feel productive [3]. Benefits that reflect stated values build trust. Benefits that contradict them erode it.
Where Most Companies Go Wrong
If alignment matters so much, why do most companies struggle? The answer usually comes down to process.
Benefits decisions typically involve HR, finance, and sometimes legal—but rarely marketing, brand strategy, or executive leadership beyond budget approval. The conversation centers on cost containment and compliance, not strategic alignment. This creates predictable problems.
Benefits happen to companies rather than being chosen intentionally. Renewals arrive, premiums increase, and the focus becomes damage control. There’s no framework for asking, “Does this still serve who we’re becoming?”
Benchmarking replaces strategy. “What do similar companies offer?” is a reasonable question, but it shouldn’t be the primary one. Benchmarks tell you what’s average. They don’t tell you what’s right for your organization.
Different stakeholders optimize for different goals. Finance wants cost predictability. HR wants competitive offerings. Legal wants compliance. Without a shared framework tied to mission, these priorities conflict rather than align.
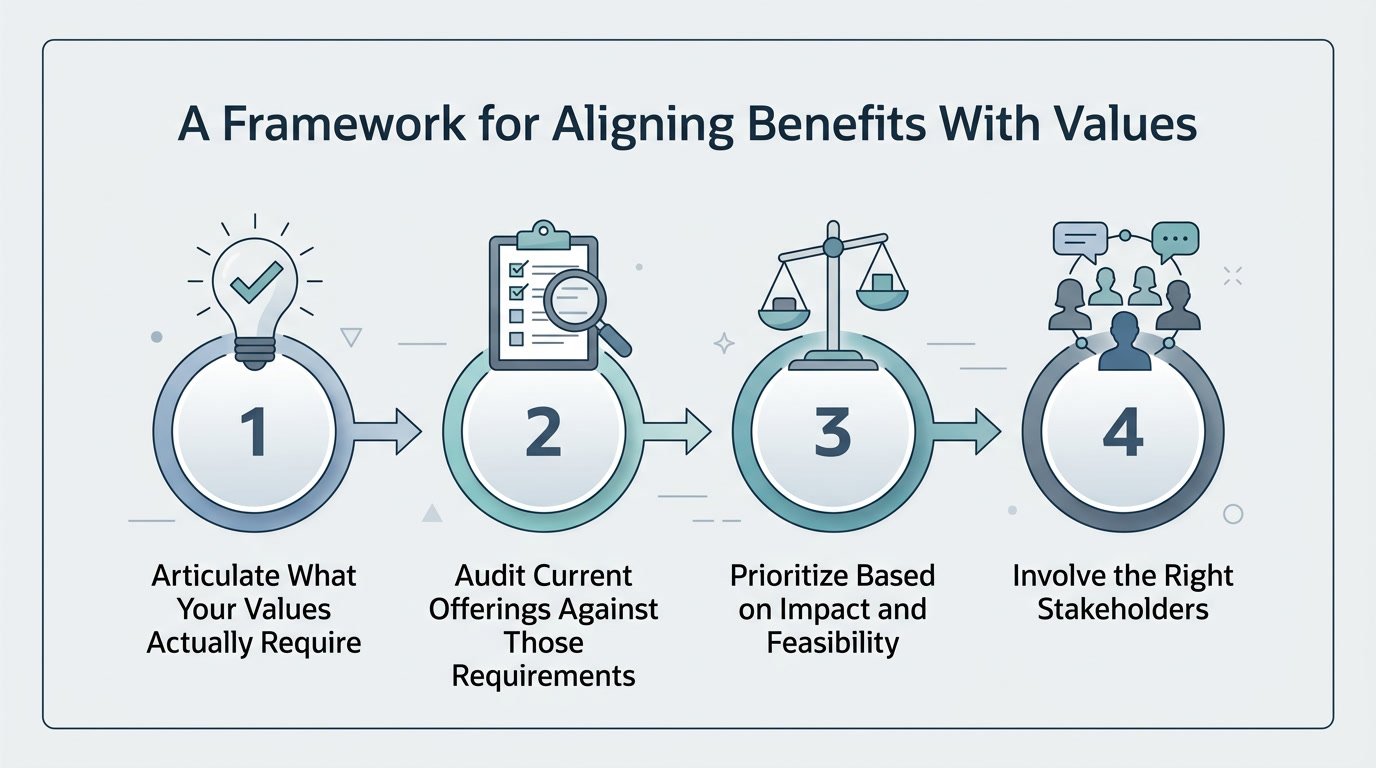
A Framework for Aligning Benefits With Values
A values-benefits audit identifies alignment, gaps, and contradictions in current offerings.
Alignment isn’t a one-time project, but it starts with a structured conversation most organizations have never had.
Step 1: Articulate What Your Values Actually Require
Pull out your mission statement and values. Now ask: what would these require of a benefits program if we took them seriously? Be specific. “We value our employees” is too vague to act on. “We believe caregivers shouldn’t have to choose between their families and their careers” gives you something to measure against.
If we say we value work-life balance, what does our PTO policy actually communicate?
If we say we invest in our people, does our professional development budget reflect that?
If we say we’re family-friendly, do our parental leave and caregiving benefits support that claim?
If we say we prioritize wellbeing, how robust is our mental health coverage?
Step 2: Audit Current Offerings Against Those Requirements
With value-driven criteria in hand, examine your current benefits through three lenses. Alignment: benefits that actively reinforce stated values—strengths to highlight in employer branding. Gaps: areas where your values suggest you should offer something you don’t—opportunities. Contradictions: benefits or policies that actively undermine stated values—urgent priorities, because they damage credibility.
Step 3: Prioritize Based on Impact and Feasibility
You won’t fix everything at once. Prioritize by visibility (which gaps are most apparent to employees and candidates), materiality (which changes most meaningfully affect employee experience), and feasibility (what you can realistically implement given budget and timing). Sometimes the highest-impact changes aren’t the most expensive. Improving mental health coverage might cost less than you expect. Adding caregiving resources could be achieved through an EAP enhancement. Flexibility policies might cost nothing but require a culture shift.
Step 4: Involve the Right Stakeholders
This is where most alignment efforts stall—the conversation stays inside HR or gets delegated to the broker. For mission alignment to work, you need voices that understand brand, talent strategy, customer expectations, and financial reality. This isn’t about adding bureaucracy. It’s about one focused conversation—ideally annually, before renewal season—that connects benefits to broader strategy.
Making Values Tangible: What to Look For
Abstract values need concrete expression. Here’s how common organizational values translate into specific benefits decisions—and where contradictions tend to hide.
“We Prioritize Employee Wellbeing”
Tangible expressions include mental health coverage with parity to physical health, preventive care incentives that respect autonomy, and reasonable out-of-pocket maximums that don’t create financial crisis during health emergencies. Red flags: high deductibles–without funding a Health Reimbursement Account or Health Savings Account–which discourage care-seeking, mental health carve-outs with limited networks, and wellness programs that create more obstacles to engagement than accessibility. MetLife’s 2026 data underscores the urgency—half of employees report avoiding medical care because of out-of-pocket costs [4].
“We Support Working Families”
Tangible expressions include parental leave that goes beyond legal minimums and applies equitably regardless of how someone becomes a parent, caregiving support for employees managing aging parents (not just childcare), dependent care FSAs, and fertility benefits that support diverse paths to parenthood. Red flags: different leave treatment for birth parents versus others, flexibility on paper but cultural pressure that penalizes usage, and no acknowledgment that caregiving extends beyond young children.
“We Invest in Growth”
Tangible expressions include professional development budgets employees can actually access, learning stipends for conferences and certifications, and student loan assistance. Red flags: development budgets that go unused because approval is cumbersome, training only available for certain levels, and no budget despite a stated commitment.
“We Trust Our Team”
Tangible expressions include remote work policies without elaborate justification, home office stipends, benefits that work across counties and state lines, and results-oriented evaluation. Red flags: remote work technically allowed but culturally discouraged, and managers who treat flexibility as a privilege to be earned.
Common Objections
“We can’t afford better benefits.” Maybe, but often the issue isn’t total budget—it’s allocation or an inexperienced broker who is not familiarized with alternative-funding options. Some high-impact alignment opportunities cost very little: flexibility policies, caregiving resources through specialty companies and EAPs, and clearer communication about benefits employees already have but don’t use.
“Our broker handles benefits. This isn’t a strategic conversation.” Your broker is an important partner, but they shouldn’t be the sole architect of your benefits strategy. Brokers operate within the options they can access and the incentives they face. The strategic conversation about alignment should happen internally first, then inform what you ask your broker to find.
“Employees just want lower premiums.” Some do, but employee preferences are more nuanced than surveys often capture. MetLife’s research consistently shows that employees value benefits that signal genuine care—sometimes more than marginal premium differences [3]. Also, candidates evaluating offers think about total value proposition, not just take-home pay.
“We’re too small for this to matter.” It matters more when you’re small. Early-stage and mid-sized companies are building culture in real time, and benefits decisions set precedents. The discipline of connecting benefits to values scales with you.
Three Actions You Can Take This Quarter
A structured 90-minute conversation can connect benefits strategy to organizational mission.
Conduct a values-benefits audit. Map your stated values to current offerings. For each value, identify what’s aligned, what’s missing, and what contradicts. This exercise alone often surfaces surprising gaps.
Schedule the cross-functional conversation. Identify three to five stakeholders who should be part of benefits strategy but typically aren’t. Schedule a 90-minute working session before your next renewal cycle.
Review your employer brand messaging. Read your careers page, job descriptions, and recruitment materials. What do they promise? Now ask: do your benefits deliver on those promises?
Frequently Asked Questions
How often should we revisit benefits alignment?
For employers with over 100 employees, you should plan for a pre-renewal meeting (or benefits assessment) approximately four months after the new year’s benefits have been in place. Small employers (i.e. under 100 employees), would do this approximately seven months after the plan year started. This will give you time to survey your organization’s engagement, understanding, and user-experiences. Additionally, your broker can start exploring ancillary plans, such as richer life and disability benefits and more voluntary plans.
Large employers would have their official renewal meeting six to five months before renewal with their broker; whereas, small employers would have the official renewal meeting three months before renewing benefits since carriers do not send out the renewal until then. This gives the broker time to research options and negotiate with carriers before enrollment. Major changes—new leadership, significant growth, strategy shifts—may warrant additional off-cycle review.
What if our values are too generic to guide benefits decisions?
That’s actually useful information. If your stated values are too vague to inform benefits choices, they’re probably too vague to guide other organizational decisions. Use the benefits conversation as an opportunity to get more specific about what your values mean in practice.
Should we involve employees in benefits decisions?
Employee input is valuable but needs to be gathered thoughtfully. Surveys and focus groups reveal which benefits matter most and where offerings fall short. Avoid promising specific changes before you know what’s feasible—but close the loop by communicating what you learned and what you’re doing about it.
Take the Next Step
If your benefits package feels disconnected from what your company stands for—or if you’re not sure how to start the conversation—Q can help you map out options and facilitate the cross-functional work that makes alignment real.
Bring us your Q. Request a consult and let’s connect your benefits program to your mission.
About Q Benefits Administration
Q Benefits Administration is a benefits infrastructure consulting firm founded by Cora Lynn Alvar (SHRM-CP), a licensed Life & Health insurance agent with over a decade of experience in mid-market benefits strategy. Q helps HR, finance, and operations leaders navigate complex benefits decisions, HR technology selection, and high-stakes transitions like PEO exits. Our approach is advisory-first: we help you make smarter decisions, build reusable frameworks, and ensure your benefits program reflects who you are as an organization.
Cited Works
[1] SHRM — “2025 Employee Benefits Survey Executive Summary.” https://www.shrm.org/content/dam/en/shrm/topics-tools/research/employee-benefits/2025_annual_benefits_survey_executive_summary.pdf. Published: 2025. Accessed: 2026-02-26.
[2] Glassdoor — “Mission & Culture Survey 2019.” https://www.glassdoor.com/blog/mission-culture-survey/. Published: 2019-07-10. Accessed: 2026-02-26.
[3] MetLife — “2025 Employee Benefit Trends Study.” https://www.metlife.com/workforce-insights/employee-benefit-trends/. Published: 2025-03. Accessed: 2026-02-26.
[4] MetLife — “New MetLife Data Finds Rising Cost Pressures Outpacing Gains in Workforce Well-Being.” https://www.metlife.com/about-us/newsroom/2026/january/new-metlife-data-finds-rising-cost-pressures-outpacing-gains-in-workforce-well-being/. Published: 2026-01-07. Accessed: 2026-02-26.